The liver and liver function are key health parameters. By contrast, higher visceral fat is related to poor organ function. The truth is that visceral fat, unlike subcutaneous fat or peripheral fat, is more relevant to health. Visceral fat deposits are known to cause systemic damage associated to diabetes, high blood pressure or cardiovascular disease. Similarly, nonalcoholic fatty liver disease is one of the most widespread diseases in the Western world (1). The main causes for the development of fatty liver are overweight, obesity and diseases related to cardiovascular risk such as diabetes, high blood pressure or high cholesterol. As we mentioned in previous posts, the risk of having a fatty liver or blood parameters related to fatty liver is the higher chance of having cardiovascular disease (2). Controlling the enzymes that regulate liver damage (transaminases) and visceral fat levels are key to the development of good health.
In this regard, the aim of this post is to analyze and transfer the success story that we have experienced at the Wiems Lab after the application of whole-body electrical muscle stimulation (WB-EMS) 3 days a week for 6 weeks in a healthy male weighing 104 kg.
Click here to read the full study on the application of WB-EMS in improving body composition in men.
To find out more about the state of liver function in the body, we took some blood the week prior to training, in week four of the intervention, and in the last week of training. Similarly, for visceral fat control, we perform a dual energy X-ray densitometry (DXA) every two weeks.
Initial assessment
As in the studies cited above, in order to be able to affirm that there have been changes after the application of WB-EMS, we must have a baseline. In this case, the baseline originated through:
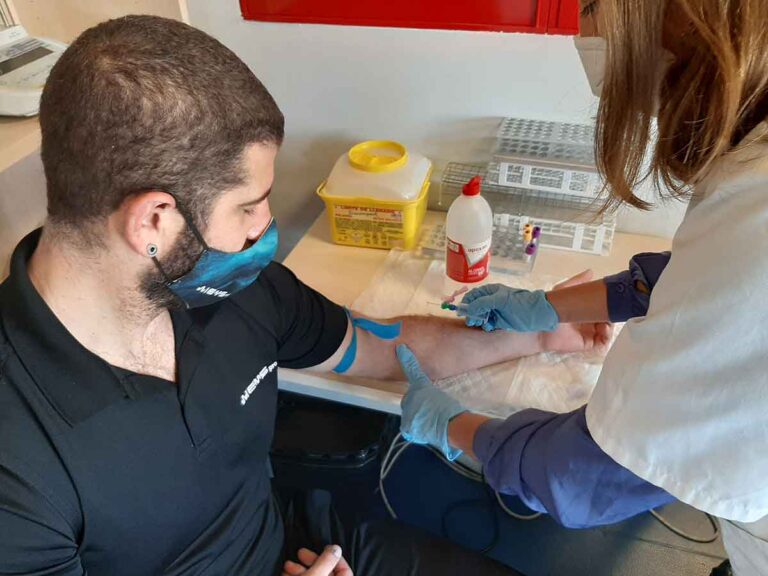
- Blood collection: We drew blood from the ulnar vein of the left arm. The collection was performed by a specialized nurse and the blood was analyzed after centrifugation. The blood was frozen at a temperature of -80ºC for preservation in order to be able to analyze other blood parameters of interest at a later date. The following blood parameters were analyzed: i) total cholesterol ii) HDL cholesterol, blood sugar and liver enzymes such as ALT, AST or GGT.
- Visceral fat (VAT): Dual energy X-ray densitometry was used to measure visceral adipose tissue. It is worth mentioning that this device is the gold standard for the measurement of bone mineral density but not for the measurement of body fat as might be the case with magnetic resonance imaging. However, it provides highly reliable data on body fat levels. Visceral adipose tissue is, as we have said, that which accumulates in the organs and poses a greater risk to health.
Training plan
To sum up, the training was divided into a day of strength training with pushing exercises, such as push-ups, squats, military presses, etc. Another day was devoted to strength training but with traction exercises such as one-handed rowing, deadlift or pull-ups. And finally, a day of high-intensity interval training with cycle ergometer and elliptical trainer. If you want to learn more, click on this link to see the load progression and the electrical programs used.
Improvements achieved
Next, we will detail the improvements achieved in this training with electrostimulation.
Liver enzymes and blood data
Before beginning the analysis, we will point out that we have 3 points in time in which blood was drawn: at the beginning of the training, at week 4 and at week 7 after finishing the training. As far as liver enzymes are concerned, this subject obtained amazing changes.
We will begin by analyzing the ALT enzyme (Alanine aminotransferase). An elevated level of this enzyme indicates possible liver damage. As we know, when the liver is overworked, this enzyme is released into the bloodstream, increasing cardiovascular risk. On this occasion, and knowing that the normative values of ALT are between 7 and 36, and in some cases 50 U/L, this male began the study with highly worrisome values: 125.06 U/L. Fortunately, the prescribed training reduced this value at week 4 to 56.20 U/L, and he ended the study with amazing values of 35.73 U/L. If we analyze these data, we see that there was a 71% reduction in this transaminase.
As we can assume, the other liver enzymes followed the same pattern. In the case of AST, it started with 120.43 U/L, and ended with 24.06 U/L with an approximate 80% reduction. Likewise, GGT decreased from 96.52 U/L to 42.70 U/L.
If we move on to other blood parameters, we see how in total cholesterol levels, this man began the study with 173.35 mg/dL, going on to have 172.13 mg/dL at 4 weeks, and ending with levels of 171.77 mg/dL. The change obtained in this variable was approximately 1%. On this occasion, we could not say that there was a significant decrease in total cholesterol.
In turn, if we turn to HDL cholesterol, we see that its initial levels were 66.97 mg/dL, at week four, it dropped to 60.19 mg/dL, and ended at 60.24 mg/dL. On this occasion, although not in a resounding way, we can confirm that there was a slight change of 10% in HDL cholesterol.
In terms of blood sugar levels, there was also a slight change in values, from close to a slight prediabetes to much more normative values. He started the study with fasting values of 99.01 mg/dL, and ended with a value of 89.72, i.e.; there was a -9% reduction in blood sugar levels.
Visceral adipose tissue (VAT)
As previously mentioned, VAT is measured both by the area it occupies and by the grams of fat it contains. This male had an initial VAT level of 602 grams and an area of 125 cm2, and ended the study with values of 408 grams and an area of 84.6 cm2. In both cases, he started with moderately worrisome values, since >400 grams of visceral fat are dangerous to health, and an area above 100 cm2 is also dangerous to health. We were able to produce a 33% reduction in both parameters, and we were able to introduce these values within the normative range for this person, sex and age.

What does electrical stimulation contribute to this process?
As we have mentioned in previous posts, it is difficult to isolate the exclusive effect of WB-EMS during this intervention process that we carried out in the Wiems Lab. The only fact we cannot neglect is that this person already had experience in electrostimulation. The fact that he had been previously exposed to this stimulus means that its effect may be somewhat less. Even so, we see in our data that the improvement achieved was astounding. The results of the procedure were excellent.
There is no doubt, on the other hand, that the subject’s adherence and the extra work of the WB-EMS brought about a substantial change in this individual.
Conclusion
The WB-EMS can be a useful tool for lowering of visceral body fat levels, and for the improvement of blood parameters related to liver function. Electrostimulation is still under continuous debate and, on this occasion, at the Wiems Lab, we can confirm that electrostimulation is useful for the reduction of visceral fat.
“WB-EMS enhances the effects of training.”
It is important to keep in mind that, far from being variables of physical change, these variables show the person’s health condition; therefore, WB-EMS is very well positioned to achieve a metabolically healthy body. We have found that cardiovascular risk values improved, and we can conclude that WB-EMS seems to enhance the effects of training.
Unai Adrian Perez de Arrilucea
Abraham Carlé Calo
Wiems Lab Team